For many individuals who have had a TBI, this blog title may resonate on many levels. Patients may be told that they look fine, or that results of cognitive or other testing are normal, yet know that they are not at their baseline. That said, the title of this short blog refers not to this overarching issue, but to one common mistake made in evaluating people with a history of concussion.
Hypothyroidism
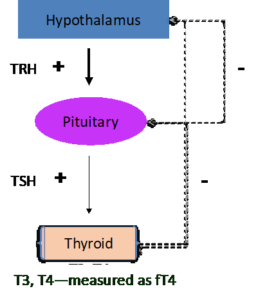
To review parts of my introductory blog (Hormone Dysfunction after Concussion), I spend my time thinking about the pituitary and its hormonal axes, including the hypothalamus-pituitary-thyroid axis. The thyroid is a gland, located at the base of the neck. Thyroid hormone works throughout the body. Hypothyroidism—insufficient production of thyroid hormone—is not an uncommon endocrine problem. Symptoms of hypothyroidism may include fatigue, weight gain, irregular periods, feeling cold, changes to hair and skin, and constipation; children may exhibit altered school performance. It is important to note that any of these symptoms may occur for a myriad of reasons, not only due to low levels of thyroid hormone.
TSH (thyroid stimulating hormone)
Hypothyroidism is most frequently due to an issue with the thyroid gland itself. This is frequently identified by the finding of an elevated thyroid stimulating hormone (TSH) level. TSH is made by the pituitary, and when a healthy pituitary senses a too-low thyroid hormone level, it secretes more TSH to help drive the thyroid gland.
Thus, an elevated TSH is a sign to check thyroid hormone levels, and, if the thyroid hormone is also low, this is often a reason to take additional (synthetic) thyroid hormone.
However: A “normal” TSH is not always normal if there is reason to suspect pituitary or hypothalamic damage or dysfunction. A damaged pituitary may not make sufficient TSH, resulting in a low level of thyroid hormone. This low level of thyroid hormone may be able to stimulate the pituitary enough to get the TSH into the usual “normal” range, but no higher. In the presence of low thyroid hormone levels (measured as free thyroxine, or fT4), a normal TSH is not normal, but inappropriately normal, and an indicator of central hypothyroidism.
Thyroid Function
I too often hear or read that a normal TSH is evidence of normal thyroid hormone. This dangerous misconception is even repeated in some publications. In situations in which pituitary damage is a possibility, both TSH and free T4 should be used to evaluate for thyroid function. Given that there is an increased risk of pituitary hormone deficiencies after concussions, testing for thyroid function (either as part of an annual screening test, or due to symptoms) should include both TSH and free T4.
A final note: If your “normal” is not your pre-concussion baseline, find a physician who understands concussion and endocrine issues and, most importantly, listens to you and can then take appropriate action. It is never inappropriate to ask questions.
For more information, check www.neuroendocrineassociates.com, or reach out to the Concussion Care Centre of Virginia, 804-270-5484 or info@cccv-ltd.com.
